Glancing at her reflection in her full-length mirror one day during her second trimester, Amy saw something she’d only ever seen on the legs of her mother and her two aunts: purplish, knotted veins just under the skin. “I thought varicose veins only happened to old people!” Amy wailed over the phone to her sister that evening.
The next day Amy paid a visit to her obstetrician and learned that varicose veins can occur in all adults, although more often in women and people over the age of 50. She also learned that varicose veins—and their milder variant, spider veins—are common during pregnancy, and usually go away on their own after the baby is born and weight returns to normal.
Varicose veins are swollen, twisted veins that are visible just under the skin. Though they usually occur in the legs, varicose veins also can form in other parts of the body. Spider veins appear in the skin as a cluster of small blood vessels that resemble a spider web. Hemorrhoids are a type of varicose vein that occur in the rectum. For many people, varicose veins and spider veins are primarily a cosmetic concern and not a cause for worry. But in some people varicose veins can cause discomfort and occasionally lead to more serious problems.
HOW VARICOSE VEINS DEVELOP
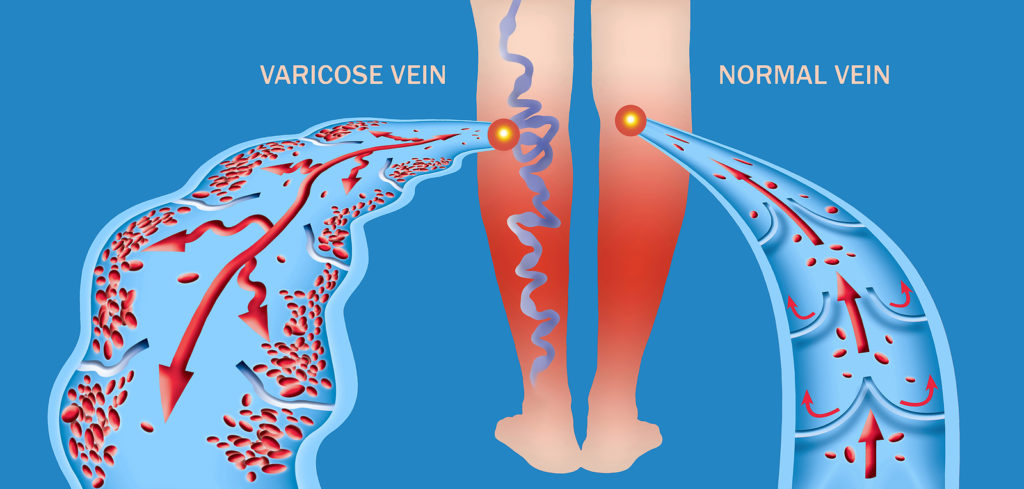
Varicose veins are often caused by weak or damaged vein walls and valves, sometimes the result of increased blood pressure that occurs during pregnancy or in people with chronic constipation, obesity or other causes. Because standing and walking upright increases the pressure in the veins of your lower body, something as simple as being on your feet for long periods can bring on a case of varicose veins. Over time, veins may grow larger and become distorted, resulting in the knotted, bulging appearance common to varicose veins. Spider veins are found closer to the skin’s surface and are often red or blue. Spider veins can also be found on the face.
You may be at increased risk for varicose veins if you:
- Are over age 50
- Sit or stand for long periods,
- Have a sedentary lifestyle
- Are overweight or obese
- Are pregnant
- Have a family history of varicose veins or deep vein thrombosis.
SYMPTOMS
Signs and symptoms of varicose veins include bulging, bluish veins; swelling, burning, throbbing or itching in the legs and feet; changes in skin color around a varicose vein; and nighttime leg cramps. Sometimes Your symptoms may worsen when you are seated or on your feet for long periods, and may improve when you lie down or put your feet up.
See your doctor if the discomfort of varicose veins starts to limit your activities. Your doctor will do a physical exam and ask you about your symptoms, family history, activity level, and lifestyle. Your doctor may order tests of your leg veins using an ultrasound, X-ray or CT scan.
COMPLICATIONS
Untreated varicose veins can lead to complications such as skin ulcers, skin color changes, and minor bleeding. Persistent bleeding from varicose veins is a medical emergency, so see your doctor right away if the bleeding from a varicose vein doesn’t stop within a few minutes.
Some research suggests that people with varicose veins are more at risk for deep vein thrombosis or a pulmonary embolism—a life-threatening condition in which a blood clot that forms in a deep vein of the body breaks away and travels to the lungs. If you have varicose veins and experience chest pain and shortness of breath, see your doctor right away or go to the nearest emergency room or urgent care center.
TREATMENT AND PREVENTION
Treatment for varicose veins is aimed at relieving the discomfort and approving the appearance of varicose veins. This may include lifestyle changes, such as losing weight or becoming more active; compression socks to help your veins move blood more efficiently; or medication to reduce blood pressure. In severe cases you doctor may recommend one of several surgical and less-invasive procedures available to remove or close varicose veins.
Other good-health guidelines that may help relieve the discomfort of varicose veins include avoiding standing or sitting for long periods, putting your feet up for a few minutes a day, and wearing non-restrictive clothing.
WORK CITED
“Are Your Varicose Veins a Sign of Deeper Trouble?” Health Essentials, The Cleveland Clinic. June 4, 2018. https://health.clevelandclinic.org/are-your-varicose-veins-a-sign-of-deeper-trouble/
“Spider Veins.” American Society for Dermatologic Surgery. https://www.asds.net/skin-experts/skin-conditions/spider-veins
“Spider Veins: How Are They Removed?” Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/varicose-veins/expert-answers/spider-veins/faq-20058284?p=1
“Varicose Veins.” Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/varicose-veins/symptoms-causes/syc-20350643
“Varicose Veins.” Medline Plus. https://medlineplus.gov/varicoseveins.html#cat_51
“Varicose Veins Overview.” National Heart, Lung and Blood Institute. https://www.nhlbi.nih.gov/health-topics/varicose-veins

 Treating and Preventing Head Lice In Children
Treating and Preventing Head Lice In Children
